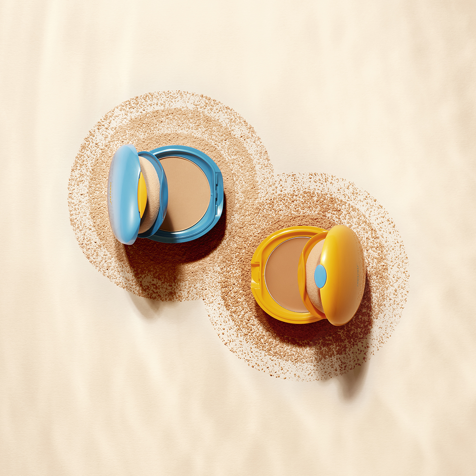Shiseido Fondotinta compatto solare Best Seller Un Make-Up che si prende cura della pelle preservandone l'idratazione con SPF6, in vacanza ed in città... | By Profumerie Piselli | Facebook

Shiseido UV Protective Compact Foundation SPF30 medium beige SP60 fondotinta compatto solare : Amazon.it: Bellezza

Shiseido UV Protective Compact Foundation SPF30 dark beige fondotinta compatto solare : Amazon.it: Bellezza